Obsessive Compulsive Disorder (OCD)
My friend’s mother-in-law has been in and out of hospital lately due to sleeping pill overdose. She takes two pills before sleeping at night and she forgets about the pills and takes another two pills in the afternoon the next day. Overtime, her heart becomes weaker, and she eventually got admitted to the hospital for weeks.
Most of the time, her family likes it when she sleeps as she suffers from OCD. She wants everything to be clean and tidy, and she will make her maid mop and sweep multiple times in a day. She wants everyone to behave in a particular way, and the house has to be set in a particular manner.
This brings me to read more about OCD and this is what I discovered.
What is OCD?
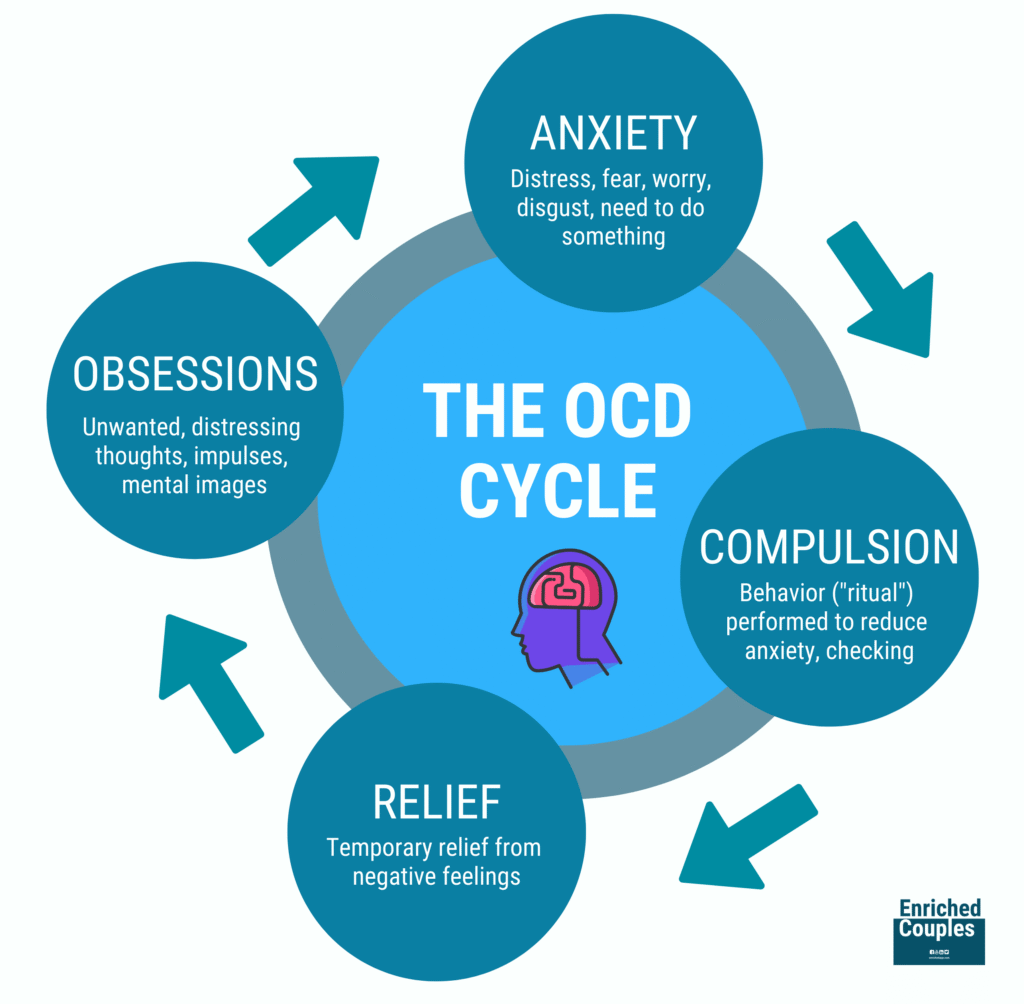
OCD stands for obsessive-compulsive disorder. It’s a mental health condition characterized by:
1. Obsessions – Unwanted, intrusive, and disturbing thoughts, urges, or images. Common examples include:
- Fear of germs and contamination
- Fear of self-harm and harming others
- Taboo thoughts (e.g., LGBT thoughts, thoughts of going for jihad)
- A need for everything to be symmetry and in order
2. Compulsions – Repetitive actions performed or looping thoughts to try to reduce the anxiety caused by these obsessions. Common compulsions include:
- Excessive nitpicking and cleaning
- Checking if items are kept safely and all doors are locked
- Counting, tapping, or mumbling the same words
- Arranging objects until the desired perfection

Whenever someone mentions OCD, many assume it is about being clean or organized. However, OCD is much more than that. It is thoughts and behaviors that are unwarranted, and many sufferers feel they are unable to stop them. These actions and thoughts can significantly interfere with daily life, relationships, and functioning.
In my friend’s case, she does not have much interaction with her mother-in-law despite staying under one roof. She also doesn’t leave her kids under the mother-in-law’s care as the mother-in-law is not in the right state of mind and has ignored her children many times.
OCD-Related Conditions

OCD is a wide spectrum of behavior. Besides the usual behavior or mannerisms listed as above, OCD can also look like:
- Body dysmorphia (bulimia, anorexia nervosa)
- Hoarding disorder
- Pulling out/eating one’s hair (trichotillomania)
- Picking at wounded skin (excoriation)
- Other kinds of picking or chewing, like nail biting (body-focused repetitive behaviour disorder)
- Consistently checking armpit and asking others about their body odour
OCD Causes

There is no definitive cause of OCD. Genetics may be the cause though no specific gene has been identified to be the trigger for this issue. It is believed an imbalance in neurotransmitters (serotonin) might be the cause.
Nevertheless, there is no correlation between stress and OCD. However, it is believed that stress can worsen OCD symptoms, especially when drastic changes are involved.
OCD may appear for the first time after a traumatic event or a life changing occurence such as a shift to another country, the birth of a sibling, childbirth, marriage or divorce.
OCD Risk Factors
OCD is a bit more common in women than in men and symptoms usually start in the teenage years. Other risk factors that may lead to this condition includes:
- A parent, sibling, or child with OCD
- Brain morphology changes
- Mental health issues like anxiety and depression
- Trauma (accident, sexual abuse)
OCD Diagnosis
In diagnosing this condition, doctors may run physical and blood tests to ensure that the symptoms are not arising from other medical conditions. This is because many psychological issues have similar symptoms with other health issues, and it can take time to make an accurate diagnosis.
There is also an OCD questionnaire to fill if the Dr suspects someone suffering it.
OCD diagnosis criteria

To actually diagnose someone with OCD, they need to fulfil all the criteria below:
- Obsessions, compulsions, or both that cannot be controlled.
- Feel forced to carry out a compulsion in response to a particular obsession, and it gives temporary relief from the stress caused by that obsession.
- Obsessions and compulsions that cripples an individual for a minimum of 1 hour a day.
- Symptoms interfere with aspects of life such as work, social life, or personal life.
- There isn’t any physical or psychological explanation for the symptoms experienced.
OCD Treatment
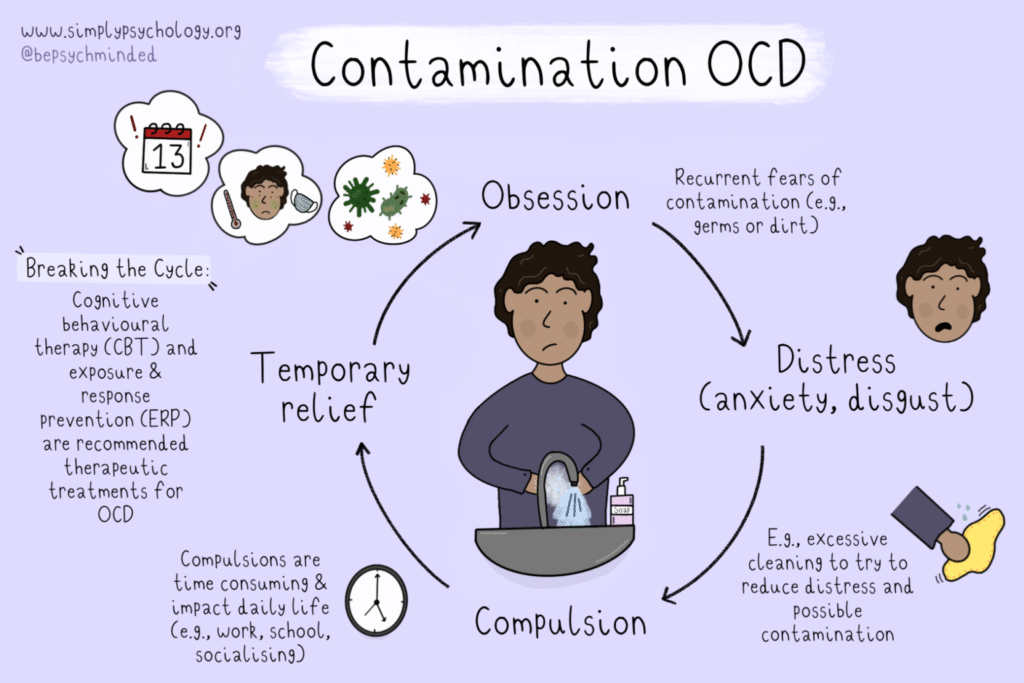
There’s no cure for OCD. However, one be able to manage symptoms through medicine, psychotherapy, or a combination of treatments.
Below are the three common methods used to manage OCD:
Psychotherapy
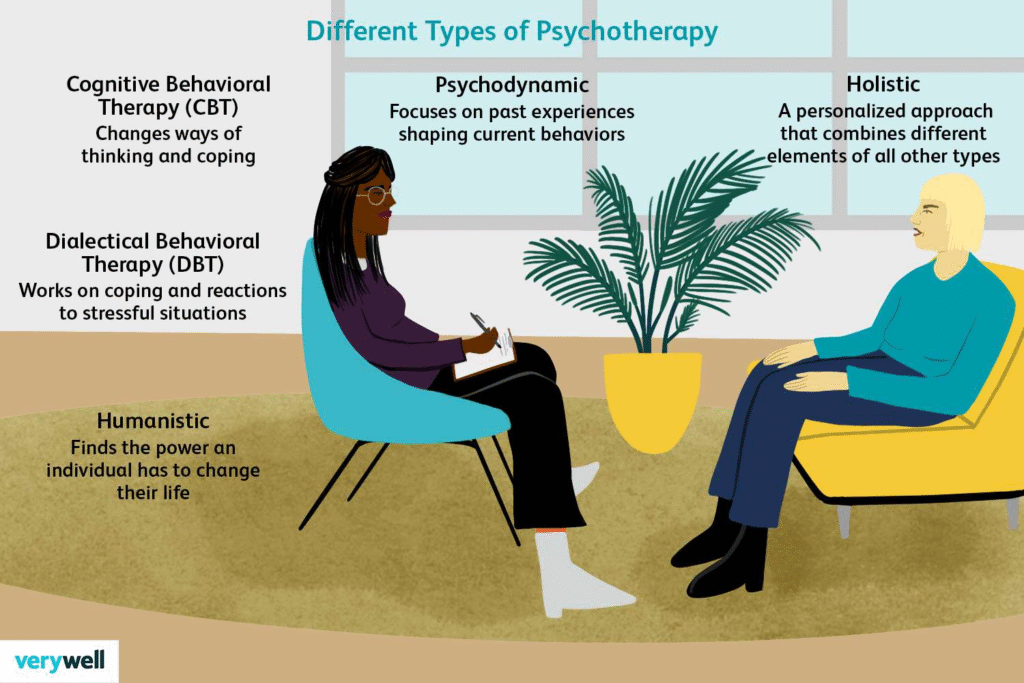
Cognitive behavioural therapy (CBT) helps with reframing thinking patterns. In a form called exposure and response prevention, doctor will put patients in a controlled situation designed to trigger anxiety or set off compulsions. With this exposure, one will learn to lessen and stop OCD thoughts or actions.
Other types of therapy used in OCD management is acceptance and commitment therapy, inference-based cognitive behavioural therapy, and mindfulness.
OCD medication

Antidepressant drugs are the main medications for OCD. They’re usually prescribed according to the severity of symptoms. Common drugs include:
- Citalopram (Celexa)
- Escitalopram (Lexapro)
- Fluoxetine (Prozac)
- Fluvoxamine (Luvox)
- Paroxetine (Paxil)
- Sertraline (Zoloft)
Once symptoms are manageable and individual have better self-control, the medicines will be tapered off accordingly.
In conclusion, by understanding the manifestation of this condition, seeking help when needed, and practicing self-compassion, individuals with OCD can work in gaining a more balanced and fulfilling relationship with themselves and those around them.







